高度に複雑化する「ストレス社会」の中で、日々の ストレス が健康に及ぼす影響は大きなものとなっています。
近年のコロナ禍などのパンデミック、AIをはじめとする高度情報化社会の影響、温暖化による気候や地球環境の変化、地震や戦争などへの不安、物価高による経済的不安など、人類をとりまく環境は過酷になっています。その中で子どもの自殺が増えるなど、ストレスの影響はじわじわと大きくなっており、医療はもとより、心理臨床や産業保健など様々な分野で、ストレスと健康の関係解明の重要性が増しています。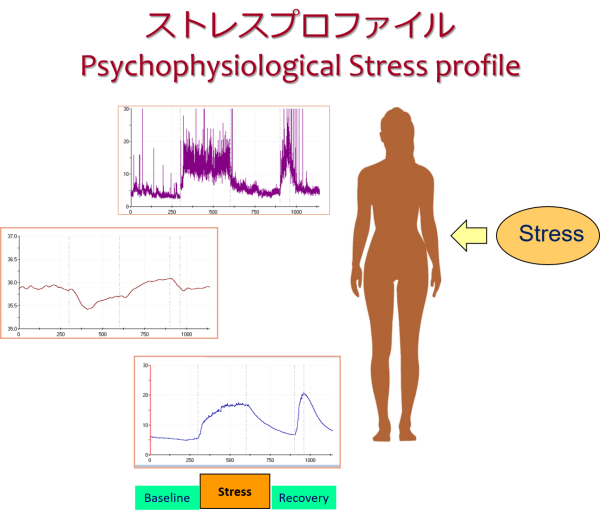
ストレスによる心身の反応については、これまでも種々の側面から検討されてきました。ストレス反応が生じても、人間の身体には回復する機能があり、「アロスタシス」(動的な恒常性)と呼ばれています。そこで、ストレスと身体機能の関係をみるには、関係性の有無や程度だけでなく、回復プロセスも含めたストレスによる変化のパターンが鍵となります。
それを踏まえて、本研究では下記の検討を行っています。
①ストレス関連疾患等における多軸的な生理ストレス反応-回復の特徴を、心理評価などと併せて検討する。
②それらのストレス反応から、種々のデータ解析手法により、臨床的に意味のあるストレス反応-回復パターンを抽出する。
③それらのパターンからストレス反応の心理・疾患モデルを構築し、新たな対象にそのモデルを適用してモデルの妥当性の検証や、疾患リスクの予測などの臨床応用を検討する。
このようなストレス反応モデルは、ストレス研究から医療、心理、産業など諸領域での応用が想定され、基盤的知見となることが期待されます。
これまでのストレス関連疾患におけるストレスプロファイルの研究から、疾患群のストレス反応には、健常群と比べて逸脱したいくつかの特徴的なパターンが存在することが分かってきました。これは、ストレス社会における人間の身体に何らかの歪みが生じている警鐘とも考えられます。 人間が本来の心身の健康を取り戻すにはどうしたらよいか、我々は、その手掛かりを心身医学の視点から探っています。
関連記事・コラム
- Stress response pattern of heart rate variability in patients with functional somatic syndromes
- 心療内科とストレス
- ストレス プロファイル Psychophysiological Stress Profile
関連プロジェクト
機械学習を用いた生理的ストレス反応のパターン分析と臨床的ストレス反応モデルの構築
https://kaken.nii.ac.jp/ja/grant/KAKENHI-PROJECT-20K03462/
[2020-2024 科学研究費補助金基盤研究C]
機能性身体症候群における精神生理学的評価と心理的評価を用いた病態の検討
https://kaken.nii.ac.jp/ja/grant/KAKENHI-PROJECT-22570228/
[2010-2012 科学研究費補助金基盤研究C]
